Lung Cancer
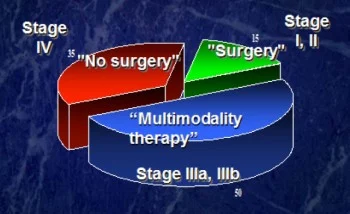
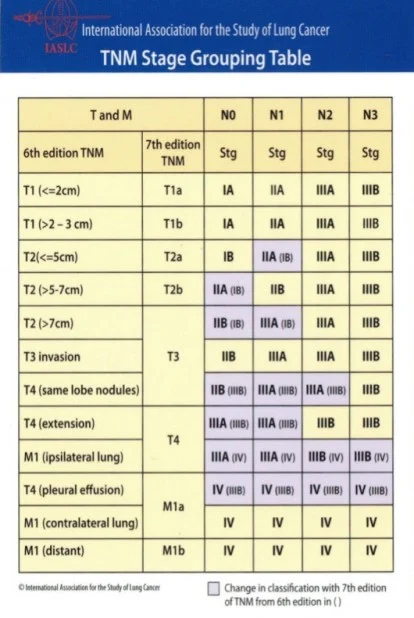
Lung cancer is a common form of cancer that starts in the tissues of the lungs. There are multiple forms of the cancer, with each requiring unique treatment plans and prognoses. Approximately 75% of patients will have symptoms from locally advanced disease at their initial physician visit. The smoking rate in the US is 24% (45 million), with 90% of lung cancers thought to be smoking related. Smoking cessation is beneficial at any age, but much greater benefit is seen in those quitting at younger ages. The risk of lung cancer does not decline for many years following cessation, making screening very important.